Knee prosthesis
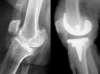
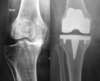
The primary total knee replacement consists of replacing the articular surfaces of the knee joint for the first time, which is in a knee that has never been implanted before the index operation. This is sort of a resurfacing concerning the femoro-tibial joint and, more inconstantly, the patello femoral joint.
What you should know before undergoing surgery
How long does it take to prepare your operation?
The operation is usually scheduled within one month after the first surgery visit. The period of one month is required in case of comorbidity (sweet, diabetes heart history...), allowing sufficient time for additional explorations if necessary. If this is not the case, the period may be shorter. The visit with the anesthesiologist (the one that will make you the anesthesia), is an obligation and should ideally take place 2 to 3 weeks before the operation.
For foreign patients, it is important that the indication of total knee replacement has already been decided and carefully designed by the patient. It is also important to organize your stay in France after the operation. When everything works well, the discharge from the clinic may be pronounced on the second postoperative day. Shorter stays are possible. However, it is important to stay nearby and consult your surgeon the following week before returning home.
Good markets and comfortable hotels are available nearby for patients and families. It is .recommended that patients be accompanied by a parent staying with him the first days at the hotel.
For patients coming from another country, it is preferable to ensure that the costs are covered by health insurance. The costs can be contained on the basis of a short-lived stay at the clinic.
For example, the clinic will ask 8000 euros for 3 nights in a private room. The cost can be reduced to less than 7000 euros for a stay of 2 nights in a double room. Anesthesiologist (1000) and the surgeon's fees (2000) are not included. Including their fees, the total cost of the operation (replacement of hip, knee or ankle primary) are of about 10000 euros.
What you should know before undergoing surgery?
This operation provides excellent functional results, including the relief of pain, with a normal and unlimited walking distance. Patients report a knee completely forgotten in about 45-50% of cases. This may seem disappointing, but does not mean that your functional result is bad in other cases. In fact, you can perceive numbness or irritations in wet weather. In contrast to the hip, the knee joint is only covered by a thin layer of skin and subcutaneous tissue, making it more sensitive to stimuli outside joint. Fortunately, these symptoms, if they exist, are moderate and don't require pain medication. That's why you should make the decision to undergo surgery only if your initial symptoms are sufficiently severe (pain, limitation of the walking distance) so that you then perceive a significant improvement. Obviously, inquire about the functional benefits provided by this operation which are very important, you restoring a normal knee said "forgotten" in 45 to 50% of cases. In the remaining cases, you feel that you have a prosthesis in certain circumstances when certain activities (ascent and descents of the stairs, running) or the change in the form of heaviness or a feeling of vise. But these potential symptoms are moderate and do not require taking medications analgesics (pain medications) term. Therefore, consider being operated on based on your initial symptoms, which must be sufficiently severe (pain, limitation of the market) so that you feel an improvement for sure. Do not expect an improvement in mobility in flexion or so she will be very moderate compared to your preoperative bending. This is indeed an effect on pain, not mobility.
How long will last the operation?
The operation lasts about an hour. You should know that the duration of the operation is not an important parameter and that it may take an hour or an hour and a half instead of an hour. This has no influence on the recovery time.
Are the operating suites very painful?
An operation of this magnitude is normally followed by pain. Everything is done to minimize the pain and make it bearable. With current technology, at wake up you will feel sort of soreness and pulling, rather related to the skin incision than to the work done in depth. The anesthesiologist adapts analgesic treatment in the immediate aftermath of the intervention. In general, the level of pain is moderate and very tolerable. A shot of Morphine may be necessary the first night. In all cases, the level of the pain decreases rapidly after the operation and becomes very tolerable in the next day, allowing the mobilization and walk in full support. Subsequently, an occasional treatment (if necessary) by Paracetamol is enough during the first month. It is desirable to not abuse of morphine, because it is a drug which is effective but which produces many side effects such as respiratory depression, digestive intolerance or urinary retention. More an addiction can be installed in case of prolonged use.
When shall I start walking?
The sooner the better to avoid Embolic complications (shutter of a vein called thrombophlebitis with its dreaded complication which is pulmonary embolism, where a piece of the clot breaks off and migrates to the lungs). The fixation of the prosthesis is strong enough to allow the immediate resumption of support and regain autonomy. Most patients get up and start walking the day of the operation. You must be helped by the physiotherapist or surgeon to perform this first stand up gradually. When the first raise, you must sit a few minutes at the edge of the bed to compose herself before standing up. The use of 2 crutches or Walker is necessary during the first stand up. The key is to control your movements so as to not to fall. The operated leg may feel overly heavy and it's normal. Initially you will need assistance to mobilize it and put you in a sitting position.
Should I do reeducation?
Yes, unlike the hip replacement, rehabilitation is necessary. It is especially important to walk and strengthen your quadriceps muscle (in front of the thigh) to be able to perform an active extension against gravity. We must quickly get active extension, i.e. be able to lift your leg from the bed by now rising the knee in extension (this is called locking the extension). It is not easy at first. You'll start by getting your knee extended as if you wanted to crush a pillow under your knee. You must see your muscle move. These contractions are called isometric and must be renewed morning noon and night. You can make these contractions on 2 sides, the side not operated causing the operated side to move by reflex way. Then when you sit at the edge of the bed or Chair, knee bent, try to extend your knee off the ground. You must also remember to raise your foot knee extended to contract your calf muscles and improve circulation of venous blood. These are sometimes exercises in plane flights in long-haul. In short you should not remain inert and perform these contractions in a repeated manner, somewhat like the "stretchin" even if it does not provoke movements of large amplitude initially.
When can I return to my home?
Usually you'll be sent to a rehabilitation centre, allowing you to have rehabilitation twice a day, morning and afternoon, and retrieve walking autonomy in a fortnight with two crutches. You will need a fortnight before you climb a few steps without the ramp. For the walk down the stairs in a symmetrical way, it will take more than a month. If your apartment is accessible by a lift, or is located on the first floor or ground floor, you should be at home at the end of the second week. If this isn't the case, it will may be longer. It is possible you back home directly from the clinic, without going into a rehabilitation center. It is important that you are not alone in the house, and you can be assisted by your wife or a parent. The direct return to your home must be prepared before the operation, ensuring that a physiotherapist is available to pick you up from the first or second day after the release.
Will I receive a transfusion?
In the majority of cases, a transfusion is not necessary. In some cases, it may be required especially if you had a preoperative anemia. In fact, the anesthesiologist that you will see before the operation will seek to correct the anemia (iron injections or EPO). But this may not be enough. In addition, if you have other diseases of cardiovascular order, no postoperative anemia cannot be tolerated and transfusion indications are wide. Transfusion is painless and has the solely disadvantage to delay your release.
What should I do once being back home?
Please contact a liberal nurse who will come to your home once a day to give subcutaneous injection of anticoagulants during 1 month, at fixed hours, weekends and holidays included. She can help you on this occasion to put on your contention stockings, which it is desirable to keep 1-2 months depending on your venous condition. Under certain conditions, injections can be replaced by oral tablets. If you are at home before the end of the first postoperative month, you should resume physical therapy to finish the job that you started in the rehabilitation center. In particular, you should practice using the stairs. In the first postoperative week, you should start trying to walk inside your apartment or House without crutches. You have to walk outside at least half an hour in the morning and in the afternoon, using crutches and comfortable shoes. You are completely free to walk longer if you want. You should quickly see that your crutches become no more useful and leave them after the first postoperative month. It is best to avoid driving a car during the first month and not to use public transport like the subway or bus. It is worth noting that your driver insurance could account that you are not in full possession of your reflex in the first month after the operation.
What kind of medical care?
In the rehabilitation center, the wound must be controlled once a week by a nurse who will also change the dressing. Stitches subside spontaneously. At any time, you will be able to join your surgeon by phone. Feel free to call if you notice a persistent seepage by the operating wound. Don't take any antibiotics. Take a picture and send it to your surgeon. He may asked you to return for a visit. If everything works well, you won't have to consult your surgeon prior to the 6 th postoperative week for clinical and radiographic control. It will then allow you to resume your normal activities, including driving. It is better that you stay and rest at home during the first 6 postoperative weeks. You will then be able to move and travel by plane or train.
How much time should you stop working?
Except professional necessity, the duration of the work stoppage is 2 months. Some independent self-employed workers wish to resume their activities as soon as possible. It is better in this case provide for sedentary work at home. Conversely some manual or force workers will request additional time before the resumption of their activities. Anyway, everything should be planned before the operation. Important appointments, contract signatures, long-distance travel must not be programmed in surgery suites. It will be time to program them and move forward them if all goes well.
How long before you resume sexual activities?
It is recommended to wait 3 weeks, avoiding the positions of the knee requiring a strong bending
What is the deadline for the resumption of the sport?
This depends of course on the sport. It takes 6 weeks which is the time of healing of the peri joint capsule. Subsequently, it must be very incremental and do not expect to recover a normal level before 6 months to 1 year. You must be especially careful to sports at risk (in altitude) and recover all of its articular amplitudes and muscle strength before exposed position. Having said that, some patients implanted with a total knee arthroplasty may achieve excellent performances, like running or jogging several kilometers.
Ultimately, how will be my knee?
Almost normal for common activities in a large number of cases. Very often you'll forget that you have an implant in your knee. But in other cases, not so rare, that 'almost' is to be considered and some unpleasant feelings may persist. It is for example a sensation of anesthesia on the lateral side (outside) of the scar, because sensory nervous branches were necessarily cut during the surgical incision that is vertical. This feeling of anesthesia takes a long time (several months or even years) to subside. You can also find that your knee is still increased by volume compared to the contralateral knee. This edema may persist for more than 6 months especially if you have a poor venous circulation and may require the port of compression stockings for several months. In little agile people or overweight, it is not uncommon that an apprehension to the walk down the stairs persists also several months with painful sensations in the front of the knee, requiring the holding of the ramp.
Knee flexion will be optimal only if it was before the intervention. Don't expect little or no addition of bending over your preoperative situation. Finally obtained maximum flexion in the best of cases with total prosthesis is around 130 ° but you cannot sit on your heels for example.
How to treat bilateral disease?
It is possible to operate both sides at the same time. An abundant literature on the subject has not demonstrated a higher rate of complications (compared to successive unilateral procedures). All patients, I later interviewed after a bilateral operation, confirmed that the pain was bearable, and don't have consumed more analgesics than patients having undergone unilateral procedures. No one regretted this choice, because they were happy not to return later for a second operation. In particular, the rehabilitation period has not doubled and was not longer than that of a unilateral procedure, because both sides are moving together. It is therefore a serious time savings. In addition, the rehabilitation of a unilateral operation, while the side contralateral pathological remains painful, is not easier. So, I suggest bilateral procedures to all those patients who complain of pain equivalent in the 2 sides. In fact, if I propose a unilateral procedure, these patients are unable to choose the first side to operate, because both sides are equally symptomatic. Bilateral procedures are also indicated in patients with a bilateral contracture in flexum. The only downside of bilateral procedures is greater blood loss, increasing the likelihood of transfusion. Therefore, it is particularly important to follow a procedure of blood savings, increasing hemoglobin before surgery, if necessary. Against persistent anemia contra indicates the bilateral procedure. Personally, I don't recommend simultaneous bilateral procedures, but prefer to operate the two sides successively in the same anesthesia. After the first side, blood loss is estimated with the anesthesiologist, and surgery is continued only if loss of blood from the first side were moderate. Patients should be aware of this interim evaluation and know that the second side will perhaps not be executed.
